
Homemade Poison
Notre Dame health experts respond to lead crisis
In early 2017, Notre Dame librarian Matthew Sisk offered his expertise in digital mapping to help a group of health and science professors tackling a public health problem: toxic lead poisoning local children.
A news report had found that children in the Near Northwest Neighborhood of South Bend had the state’s highest levels of lead in their blood. Sisk signed on to further refine the mapping and analysis of the state’s lead test data.
What he learned in just a few weeks prompted him to get his 1-year-old daughter, Laurie, tested for lead. Her results were below the state threshold for action, but still alarming for any first-time parent. Elevated lead levels can lead to serious cognitive, developmental and behavioral problems in children, ranging from hyperactivity to lower IQ.
“I was very committed to the project from the beginning, but suddenly it was personal,” Sisk said. “There’s no safe level of lead, so it’s a little scary.”
“I was very committed to the project from the beginning, but suddenly it was personal...”
Sisk’s first reaction was “judicial panic” that included reading everything he could about lead toxicity and hastily repainting the walls in his 1875 home. He reached out to the county health department, then waited weeks for a home lead test and months for the report results.
“We realized that this was a weak point where we could help,” Sisk said. “We could develop a home test and better turnaround that can really help the panicked parent.”
The “we” Sisk refers to is the Notre Dame Lead Innovation Team, a multidisciplinary group that includes himself and four other Notre Dame professors, plus help from dozens of graduate and undergraduate students, who are developing a systematic infrastructure to address the county’s lead problem. The team’s work in the last two years has already prompted greater public awareness of the issue and accumulated six grants to fund research and solutions.
Notre Dame Lead Innovation Team’s top priority now is to develop an inexpensive but thorough lead test kit that homeowners can use to identify any danger before their children are poisoned.
“This is a more proactive citizen-science model,” said Marya Lieberman, an team member and chemist who specializes in developing low-cost analytic tests to catch fake drug products. “Rather than learn about lead problems from where kids get sick, this new model flips that paradigm. Let’s test before kids get sick.”
Current options for home lead testing are limited or expensive. A hardware store test kit costs just $10 but is limited to paint, and only light-colored paints. The results indicate a positive or negative for lead presence, but say nothing about levels. Complete home tests — analyzing paint, dust, water and soil — from private companies can cost $300 or more.
“Rather than learn about lead problems from where kids get sick, this new model flips that paradigm. Let’s test before kids get sick.”
Or homeowners whose children have already tested positive for lead can wait months, like Sisk did, for the cash-strapped county health department to produce a report.
The lead test kit that the Lead Innovation Team is developing guides homeowners in how to collect samples: three soil, three dust and two paint. Unlike the recent crisis in Flint, Michigan, water is not considered a primary lead source in South Bend. The homeowner can send in the samples for analysis and get results within three weeks. The team spent the summer testing the ease of use and reliability of the kit.
“We started by trying to test as many homes in the affected neighborhoods as we could,” said Heidi Beidinger-Burnett, an expert in public health and assistant professor in Notre Dame’s Eck Institute for Global Health. “We quickly realized we couldn’t scale up to the level of the problem even in our county. So we turned to this do-it-yourself kit. The ultimate goal is to create a better testing model for the state and maybe even the country.”
***
Old homes with peeling and deteriorating paint present a risk of lead contamination even though the heavy metal was phased out of paint and gasoline in the late 1970s. All houses built before the ban could have lead-based paint that peels and chips, creates dust and flakes into soil, but the risk is magnified in poorer areas where money for renovations is scarce.
The lead problem in St. Joseph County isn’t new. It rears its head every 15 or 20 years and gets addressed temporarily, and then funding slowly dwindles until a new panic ensues. Testing had dropped from more than 3,000 children in 2011 to about 650 kids in 2015. The latest eruption started in late 2016, when a state study that analyzed a decade of lead testing broke down the results by census tract for the first time.
More than 36 percent of the kids tested in one census tract in the Near Northwest Neighborhood had elevated levels of lead in their blood. The Centers for Disease Control and Prevention (CDC) considers blood lead levels at 5 micrograms per deciliter or above to be elevated.
To put the Near Northwest situation in perspective, the CDC estimates that about 2.5 percent of kids nationwide have elevated levels. In the year after the water crisis in Flint, 5 percent of kids tested there had high blood levels.
County health officials, under state pressure to follow new CDC limits that lowered the lead level threshold for case management, recognized they could not handle the increasing numbers and turned to Notre Dame for help.
Beidinger, who also serves on the county health board, created a class in the spring of 2017 to research the causes of the high lead levels in the Near Northwest and guide the health department’s response. That effort expanded into the creation of the Lead Innovation Team, which brought her together with Sisk and Lieberman, as well as Michelle Ngai, a visiting professor in the Eck Institute, and Graham Peaslee, a nuclear physicist.
The team did home tests in the Near Northwest in the summer of 2017 with two different methods. A field test used an X-ray fluorescence (XRF) scanner that looks like a space-age gun to instantly evaluate paint or soil. A lab test consisted of a plastic bag with rubber gloves, wet wipes for dust samples and small plastic bags for dirt and paint samples.
Each method had advantages and disadvantages. The field test was instant, but it would be difficult to scale and did not include dust, a major source of lead exposure. The lab test was more complete but took longer because samples would be individually analyzed later in a lab.
“We learned where we’d expect to find lead, so we were able to zero in on the places most likely to have lead: driplines in soil, window sills, peeling paint and places that don’t get dusted often,” Beidinger said. “So that’s what we focused this kit on. We want to put preventive measures in the hands of homeowners right away.”
Once the team decided to create a homeowner test kit, they initiated a design and development process like any other new product. Beidinger used some of her grant money from Green & Healthy Homes Initiative, a national nonprofit focused on lead safety, to hire an industrial design student, who created a pilot test box with pre-labeled sample bags and detailed instructions for collection taped to the underside of the lid.
Last summer the Lead Innovation Team distributed the box to nearly 50 homes, divided into three time periods. More than 90 percent of homes built before 1950, when lead levels in paint were reduced, had at least one positive result. Half of the homes built between 1950 and 1978, when lead in paint was eliminated, tested positive. None of the homes built after 1978 had any lead.
The tests took an average of 22 minutes for each homeowner. Students trained in taking samples observed the homeowners to ensure they followed instructions. The students also used the XRF analyzer to test each sample site. A separate lab team, deliberately blinded from the field test results, analyzed the collected samples.
When the results of the two blind tests were compared, the correlation was more than 90 percent.
“People liked the kit,” Beidinger said, “and the reliability level was really strong.”
Kathy Schuth, director of the Near Northwest Neighborhood organization, volunteered to have her home, built in 1900, tested to help ND Lead Innovation Team develop its product. Some homeowners, especially landlords of rental homes, are reluctant to do lead tests because positive results would have to be disclosed to tenants or when the property is sold.
“I expected my home to have lead paint,” said Schuth, a ’99 alumna of Notre Dame’s School of Architecture. “I figure it doesn’t matter if I acknowledge the problem or not because the home was built before 1950. The safety knowledge is way more valuable to me than the resale value.”
She was surprised, however, to find how easy it was to locate potential problem areas. She pointed to a small ding on the living room doorframe, which exposed the original varnish with a high lead level. Also, she said dust swabs in her window frames pulled up obvious paint particles despite being recently cleaned.
As association director of the neighborhood most affected, Schuth has learned plenty about lead exposure and remediation. Her association has hired three part-time workers to canvas the entire neighborhood and provide information about lead issues and testing children’s blood levels.
“The lead test kit is hugely exciting,” Schuth said. “It can be difficult to get the most vulnerable tenants to test. The ability to have that kind of testing for a reasonable price is phenomenal.”
The tests of the test kit led to a third design, which will improve the instructions and professional look, and include links to a University website with instructional videos, as well as prevention and remediation information.
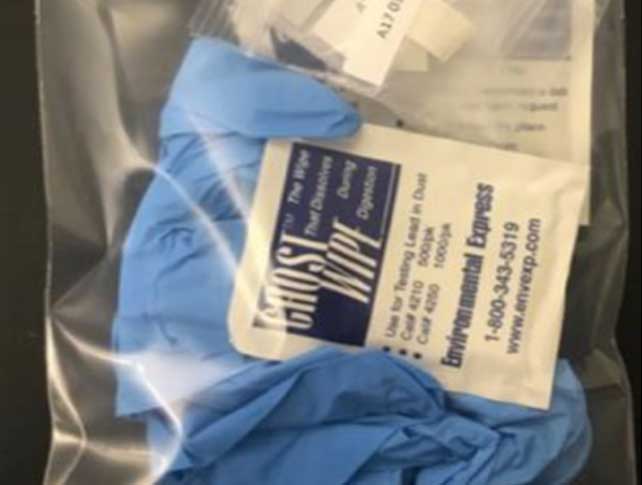
The 2017 version of the kit contained a plastic bag with rubber gloves, wet wipes for dust samples and small plastic bags for dirt and paint samples.

Upgrades to the 2018 kit include a pilot test box with pre-labeled sample bags.

The kit's future design will improve the instructions and professional look.
Crucially, the new box design will allow automated scanning of the samples for quicker results. A factory in Elkhart will produce an initial run of 200 test kits. Those will cost about $10 to produce, but grant money will make them free to users.
Sisk said the initial goal is to create a product that academic and nonprofit groups can use for lead tests. The group’s first impulse, he said, was to make it free, but Lieberman’s experience with drug tests in Africa convinced them that commercialization can be a useful way to ramp up scale and make a low-cost product more widely available. The latest test run could lead to thousands of kits distributed across the county, with a potential for commercialization to make the invention spread across the state and beyond.
Since learning about ways to mitigate lead contamination, Sisk said his daughter Laurie’s blood levels have dropped from 4 milligrams per deciliter to 1. He admits that he became a little obsessed with the topic and annoyed many of his friends talking about it.
But he said working with the Lead Innovation Team to flip the paradigm on the lead problem has been a personal palliative. The project allows him to utilize his skills to analyze and map the data, and it aims to create a new product that can help families like his — hopefully before there is a problem and a panic.
“It’s not very efficient to wait for the county blood tests to see where kids have elevated levels of lead,” Sisk said. “It’s also unethical to wait until we find out who’s affected. It’s using kids as the canary in the coal mine.”